Lung ultrasound
Lung ultrasound allows us to narrow down differentials: It can be used to rule out pneumothorax, confirm the presence of pneumonia, main stem intubation, diaphragmatic paralysis, interstitial lung disease as well pleural effusion. We begin by learning what the normal looks like under ultrasound.
Showmethepocus.com contextualizes this section by following the link here:
Introduction
When scanning the chest with ultrasound the sonographer is not actually seeing very deep. This is due to the high acoustic impedance which leads to a pattern of repeating horizontal lines. It is thus very difficult to see through deeper structures because of the presence of air in the lung. What we do see though is several artifacts that the ultrasound machine interprets are coming from tissues. When a disease process reduced the amount of air within the lung, ultrasound findings have predictable features. When scanning the lung, the pleura must be involved in the process for it to be see on ultrasound. However clinically relevant processes do involve the pleura and can be seen: pulmonary edema, pneumonia, pleural effusion since these extend to the periphery of the lung.
Anatomically, the structures that we are analyzing with ultrasound are superficial. On the right a recap of the anatomical structures of the chest wall interrogated with lung ultrasound.

Normal pleura and related anatomic structures for reference. Image from Foresight ultrasound. These are the components of the 'Bat sign' explained below.
A linear high frequency probe (5-13MHz) may be adequate enough to analyze superficial structures such as the pleural interface of the lung and give optimal resolution. Other probes used to interrogate the pleural space include the curvilinear probe (1-8MHz) that allows the sonographer to visualize deeper structures at the expense of resolution. Even phased array transducers used in cardiac imaging (2-8MHz) can be used to view pleural space.
Scanning should occur in a longitudinal plane with the probe held perpendicular to the surface of the skin. Multiple sites should be chosen and scanning should proceed in a predetermine sequence. A comprehensive evaluation under lung ultrasound involves scanning of eight lung zones.
Equipment and Technique:
AAL
PSL
PAL
1
3
2
4
I
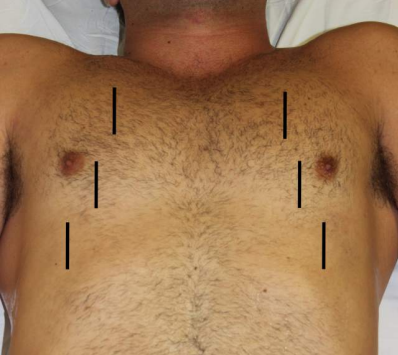
Suggested examination windows for a fast lung evaluation. A comprehensive evaluation involves scanning 8 lung areas and four of these is depicted on the image. Areas 1 and 2 denote the upper anterior and lower anterior chest areas, respectively. Areas 3 and 4 denote the upper lateral and basal lateral chest areas, respectively. PSL parasternal line, AAL anterior axillary line, PAL posterior axillary line.Image from Foresight ultrasound.
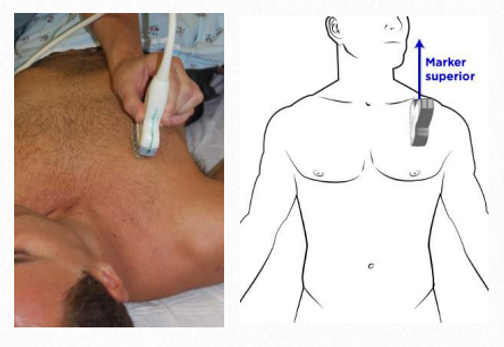
Optimal probe position examination. Notice that the probe is at 90 degrees from the skin and on the short axis of the rib which known as the longitudinal view. Image from Foresight ultrasound.
Normal Sono anatomy.
The following sonographic findings are considered normal when interrogating the lung.
Pleural Sliding
The presence of pleural sliding is the most important finding in normal aerated lung. The sonographer should visualize the hyperechoic pleural line in between two ribs moving or shimmering back and forth and represents the movement of the parietal and visceral pleura. What happens if you suspect pneumothorax and you see this finding instead? The negative predictive value for lung sliding is 99-100% for pneumothorax and thus it's presence rules out a pneumothorax. However multiple windows will have to be interrogated to rule out this diagnosis.
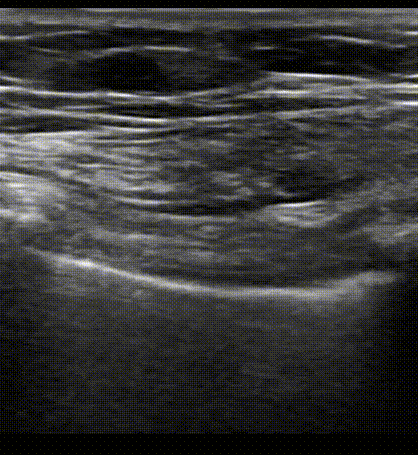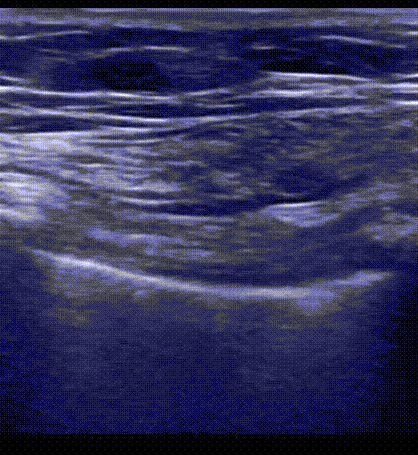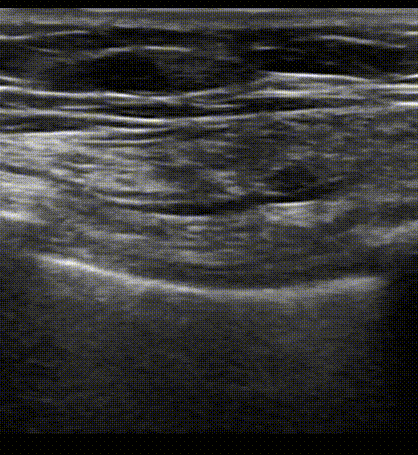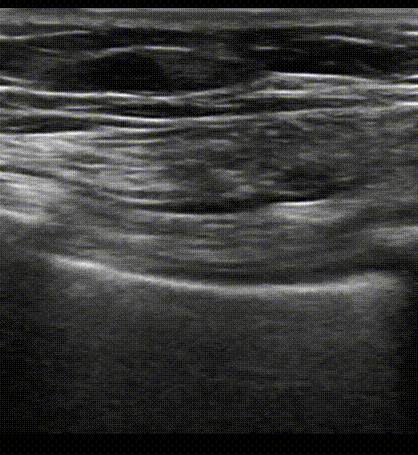
Pleural sliding as visualized on B mode ultrasound. We are seeing the 'Bat sign' in this clip. The probe has been placed on a longitudinal view of the anterior chest and the plane is cutting on the superior and inferior rib (bat wings) as well as the soft tissue that lies in between each rib space. Notice hyperechoic back and forth movement of the pleura at this interspace. The ribs at either side of the clip are creating acoustic shadows on the lung pleura which is why there is no echoes at this point.
M Mode
Lets see what happens when you use M mode on that same clip above. M mode is an ultrasound feature that allows the interrogation of sound waves along a specific scan line. The motionless portion of the chest above the pleural line creates horizontal ‘waves,’ and the sliding below the pleural line creates a granular pattern, the ‘sand’. The resultant picture is that of seashore sign.
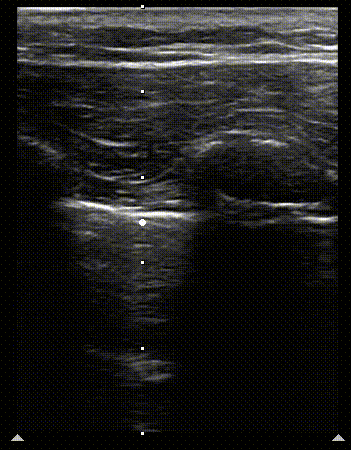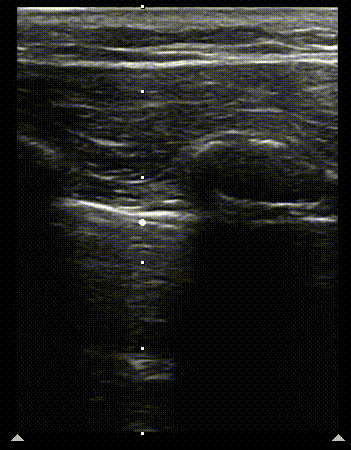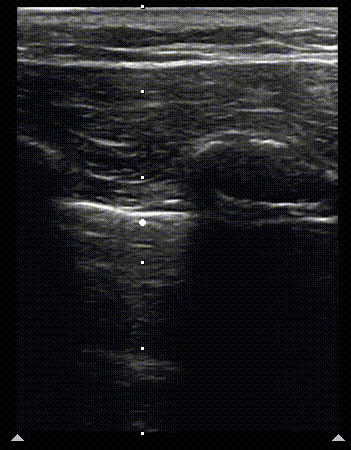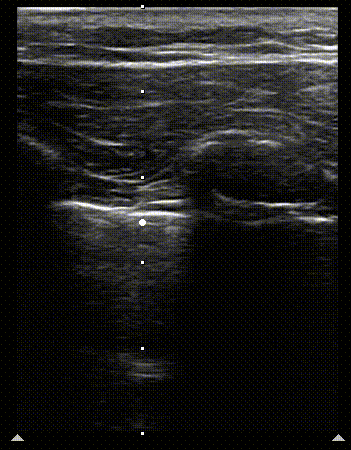
1

2
Normal M mode of the lung. Clip 1 shows the scan line being set up and still image 2, when M mode scan is turned on. The image on the right shows the seashore sign. The arrowhead marks the interface of sea (above) and shore (below) on the image.
B-lines
B-lines are reverberation artifacts that appear as hyperechoic vertical lines that extend from the pleura to the edge of the screen without fading. These are vertical in orientation. A few B-lines less than or equal to 2 in each interrogation zone is considered normal. These lines move in synchrony with lung sliding.

B lines present on this phased array scan sector. These hyperechoic vertical lines extend beyond the pleura and cover all the sector.
Lung Pulse
Lung pulse is the rhythmic movement of the pleura in synchrony with the cardiac rhythm. Its presence indicates that the parietal and visceral pleura oppose one another, and so its presence rules out a pneumothorax. To visualize a lung pulse have your probe interrogate the pleura close to the sternum where the internal thoracic artery lie.
Lung Pulse. The pleural line is moving more than 60 times/min

Comparison: lung sliding vs lung pulse
Lets compare lung sliding with lung pulse so that we get better visual picture. We will revisit these images again in the pneumothorax chapter.


Lung sliding vs pulse. On the left, we appreciate the movement of the pleural line with respiration. On the right, the pleural line seems pulsating at a rate of 70 bpm. Both of these ultrasound findings exclude a pnuemothorax.
Z lines
Z lines are short vertical comet tail artifacts that do not extend more than 3 cm from the pleural interface. They appear as shorter forms of the B lines.
Z lines coming in and out of view. See marker on the image

Lung Curtain
On this clip we see the diaphragm displacing the abdominal contents to the right with each breath. We see two ribs causing acoustic shadows. On the left we appreciate faint B-lines. Between the rib shadow we appreciate the pleural line moving down. With each breath this line moves down and causes an acoustic shadow over the diaphragm so that it cannot be seen at the end of inspiration.

Lung curtain artifact. The pleural sliding starts at the rib marked on the left arrow and extend to the second arrow on this clip, obscuring all structures that lie deeper. Notice that you can visualize the diaphragm (blue arrow) initially but then it disappears from view.
References for the LUNG chapter including pathology:
1. Gargani L, Volpicelli G. How I do it: lung ultrasound. Cardiovasc Ultrasound. 2014;12:25. Published 2014 Jul 4. doi:10.1186/1476-7120-12-25
2. Volpicelli G and all. International evidence-based recommendations for point-of-care ultrasound. Intensive Care Med. 2012 Apr;38(4):577-91.doi: 10.1007/s00134-012-2513-4. Epub 2012 Mar 6.
3. Mayo, P.H., Copetti, R., Feller-Kopman, D. et al. Thoracic ultrasonography: a narrative review. Intensive Care Med 45, 1200–1211 (2019). https://doi.org/10.1007/s00134-019-05725-8
