Ocular Ultrasound
Introduction
The assessment of ocular trauma, acute vision loss and evaluation of increased intracranial hypertension traditionally revolves around methods that are able to examine deep structures in the eye. This includes a dilated fundoscopic examination with slit lam exam and other non-invasive modalities including CT and MRI with their associated radiation exposure. Ultrasound can be used as an alternative to these with the added benefit of being a bedside evaluation, ease of use, low cost and lack of ionizing radiation.
Anatomy of the eye
We first examine the morphology of the eye so that we have a better understanding of how to interrogate the eye with the use of ultrasound.
The globe is made up of 3 layers. The sclera and cornea make up the external layer. The uvea makes up the middle layer; the choroid plexus, ciliary body and iris originate from this structure. The choroid forms the vascular layer between the sclera and the retina. The iris divides the anterior from the posterior chamber. The lens is suspended in the vitreous body by the ciliary muscles. Finally the inner most layer is the retina which is attached at the optic disc and the ora serrata. It is the intraocular pressure that hold the retina in place.
Light passes through the cornea, aqueous humor, in the anterior chamber, the lens, and the vitreous body before reaching the retina.
The optic nerve, central retinal artery and vein travel together in the ophthalmic sheath which contains cerebrospinal fluid and is a continuation of the subarachnoid space.

Schematic diagram of the right human eye on transverse section. Image by Rhcastilhos and Jmarchn.
Equipment and Technique:
The eye is a superficial shallow structure that is well positioned to be evaluated under ultrasound. Use a linear high frequency probe (13-6Mhz). An absolute contraindication to this technique includes an open globe injury.
Consider the use of a clear plastic film placed over the eyelid of the globe you are attempting at interrogating. Use copious amount of ultrasound gel over this film to minimize the amount of pressure exerted on the globe. First interrogate in a transverse orientation. You can tilt the probe in the craneocaudal direction and then have the patient look up and down with the probe stationary. The exam can then proceed in a sagittal plane with the probe tilting from left to right and then asking the patient to move the eye from left to right while you keep the probe stationary. Importantly to examine the optic sheath you must be in a transverse orientation and the probe should be rocked laterally. Remember to anchor your hand in the patient's face to have adequate control of the pressure you are applying to the eye.

1


2
3
Interrogation of the right eye and ultrasound probe movements. Image 1 depicts a transverse view. The sonographer should rock the probe up and down and then ask the patient to move the eyes up and down while the probe remains stationary. Image 2 depicts a sagittal view. The probe is rocked right and left and then the patient moves their eyes left and right while the probe remains stationary. Image 3, the probe is stationary and in a transverse position and tilted nasally to look at the optic nerve sheath. Arrows depict the rocking direction which is the direction of movement the tail of the probe while the surface that contacts the skin remains still.
Sonographic anatomy of the ocular globe and measurements
Lets have a closer look at the corresponding images that we get with those scanning planes in mind and examine the components that we can examine when interrogating the globe.
The following B-mode clips represent normal ocular ultrasound findings. On the right, an overlay of the structures that we observe.


Saccadic eye movements and optic nerve sheath
On the left, B-mode clip representing normal saccadic eye movements. Notice no free floating artifacts within the globe. On the right the optic nerve sheath (in blue) and within it, the optic nerve (in magenta).


Estimating intracranial pressure
The sheath around the optic nerve (ONS) is a continuation of the dura. A rise of intracranial pressure would thus be transmitted to the optic sheath. This results an increased ONS distention eventually leading to papilledema. Ultrasound measurement of the ONS diameter a distance of 3mm away from the retina can be used to classify patients as having increased ICP. In adults, a ONS diameter 0.5 or less is normal. One measuring greater than 0.6cm corresponds to high intracranial pressure (ICP) and correlates to an ICP>20mmHg.
To use ONS diameter to estimate ICP it is important to measure a distance from the retina (3mm) and then measure the diameter of the ONS. A value greater than 5mm suggest increased ICP.


3mm from retina
<5mm diameter
Pathology seen with Ultrasound
In the following section we will examine pathologies that can be seen with ultrasound. First, we can use ultrasound to help us differentiate between retinal and vitreous detachment or hemorrhage as a cause of painless vision loss.
Retinal detachment
Retinal detachment is a cause of painless partial or complete vision loss.
On US we appreciate an hyperechoic mobile membrane floating in the posterior chamber that is tethered to the optic nerve. It is this tethering that helps differentiate it from vitreous detachment which is also a cause of painless vision loss.
Retinal detachment can also occur in the setting of trauma

Normal US findings

Retinal detachment
Vitreous Detachment and Hemorrhage
Vitreous detachment and hemorrhage are causes of painless partial or complete vision loss.
Posterior vitreous detachment produce a hyperechoic membrane that is not tethered to the optic disc.
Vitreous hemorrhage presents with heterogenous echogenicity as a 'snow globe' effect with eye movement.

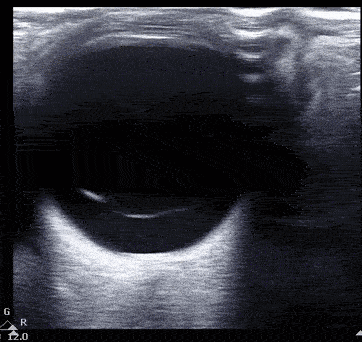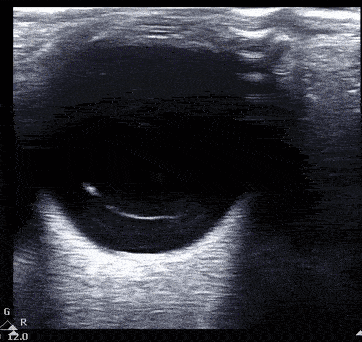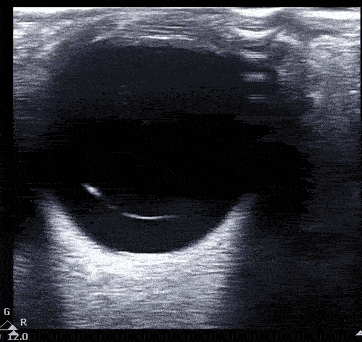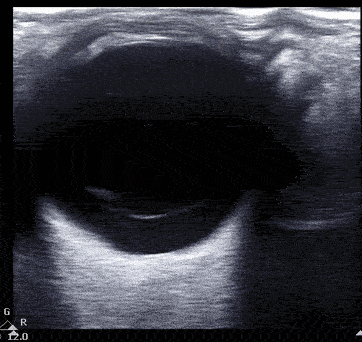
Vitreous hemorrhage
Vitreous detachment
Lens Dislocation
Presents as decreased vision and a normal pupillary reflex.
On ultrasound interrogation there is a posteriorly displaced lens.

Normal findings.

Lens dislocation.
Increased intracranial hypertension
We can observe bulging of the optic disc. This represents papilledema is it is accompanied with an increased ONS diameter greater than 6mm We can also measure the optic nerve sheath diameter. A ONS <5mm is normal while a diameter greater than 6mm is correlated with an increased ICP.


Normal findings.
Papilledema
References
-
Rajajee V, Vanaman M, Fletcher J.J, et al. Optic nerve ultrasound for the detection of raised intracranial pressure. Neurocrit Care 15, 506–15 (2011).
-
Lorente-Ramos RM, Armán JA, Muñoz-Hernández A, Gómez JM, de la Torre SB. US of the eye made easy: a comprehensive how-to review with ophthalmoscopic correlation. Radiographics. 2012 Sep-Oct;32(5):E175-200. doi: 10.1148/rg.325115105. PMID: 22977037.
-
Blaivas M, Theodoro D, Sierzenski PR. A study of bedside ocular ultrasonography in the emergency department. Acad Emerg Med. 2002 Aug;9(8):791-9. doi: 10.1111/j.1553-2712.2002.tb02166.x. PMID: 12153883
-
Kilker, B. A., Holst, J. M. & Hoffmann, B. Bedside ocular ultrasound in the emergency department. Eur J Emerg Med 21, 246–253 (2014).
-
Gandhi K, Shyy W, Knight S, Teismann N. Point-of-care ultrasound for the evaluation of non-traumatic visual disturbances in the emergency department: The VIGMO protocol. Am J Emerg Med. 2019 Aug;37(8):1547-1553. doi: 10.1016/j.ajem.2019.04.049. Epub 2019 May 11. PMID: 31130372.
